Table of Contents
Understanding Foot Pain in Bloomingdale, Illinois
Foot pain in Bloomingdale, Illinois, affects countless adults and seniors, disrupting daily activities from walking neighborhood paths to enjoying family gatherings. At Advanced Pain & Spine Management, we see many patients struggling with this lower extremity discomfort in Bloomingdale, where sedentary lifestyles and an aging population contribute to its prevalence. Studies indicate that up to 25% of midwestern U.S. communities experience chronic foot issues, often multifactorial in origin.
This localized foot discomfort can stem from local problems like plantar fasciitis, an inflammation of the tissue along the foot’s bottom, or heel pain from overuse and poor support. It may also refer from spinal conditions such as sciatica or spinal stenosis, sending pain signals down the legs. These causes impact mobility, leading to reduced independence and quality of life for our patients in Arlington Heights and Bloomingdale locations.
When simple remedies fail and symptoms persist beyond a few weeks–especially with numbness, swelling, or interference in routine tasks–it’s time to seek specialized care. We offer individualized pain treatment plans featuring minimally invasive options like targeted injections and coordinated physical therapy to restore function without surgery.
Patients often share positive experiences in our bloomingdale pain management reviews, highlighting relief and compassionate support. But what exactly causes this discomfort, and how can advanced interventions help?
Fundamentals of Foot Pain Causes
At Advanced Pain & Spine Management, we often see patients experiencing foot pain in Bloomingdale, Illinois, seeking relief from discomfort that disrupts daily activities. Understanding the fundamentals of these issues is crucial, as foot pain can stem from local problems within the foot itself or referred sources originating from the spine. Distinguishing between these helps patients recognize when simple self-care might suffice versus when professional intervention, such as at our bloomingdale pain clinic contact, becomes essential for effective management.
The foot’s anatomy plays a key role in pain development. The plantar fascia, a thick band of tissue running along the bottom from heel to toes, supports the arch and absorbs shock during movement. Surrounding structures include the heel bone, or calcaneus, prone to spurs or bursitis, and a network of nerves branching from the lower spine. When these elements become inflamed or compressed, pain arises, often exacerbated by Bloomingdale’s active lifestyles involving prolonged standing in retail or service jobs. This foundational knowledge empowers individuals to identify early warning signs and pursue timely care.
Local causes of foot pain directly affect the foot’s structures. Plantar fasciitis, an inflammation or degeneration of the plantar fascia, impacts about two million people annually, according to the American Academy of Physical Medicine and Rehabilitation (AAPM&R). It commonly results from repetitive strain, tight Achilles tendons, or excess weight, leading to micro-tears in the tissue. Heel pain often accompanies this, stemming from bursitis or bone spurs at the calcaneus insertion point. In our practice, we note higher incidences among those with occupational demands like standing for hours, common in local Bloomingdale workplaces.
- Morning stiffness: Intense discomfort upon first steps, easing with movement but recurring after rest.
- Sharp heel pain: stabbing sensation during weight-bearing, sometimes with arch discomfort or sole tenderness.
These symptoms highlight the need for prompt attention to prevent progression to chronic issues.
To aid in identification, the following table compares common local versus referred causes of foot pain, drawing from AAPM&R data on musculoskeletal conditions and midwestern prevalence studies:
| Cause Type | Examples | Symptoms | Prevalence in Bloomingdale |
|---|---|---|---|
| Plantar fasciitis, heel pain | Inflammation, strain | Morning stiffness, sharp heel pain | 40% of cases |
| Sciatica, spinal stenosis | Nerve compression | Burning, tingling in foot | 30% of cases |
This comparison underscores how local issues typically involve mechanical strain, while referred pain signals nerve involvement. Distinguishing them matters for treatment selection, as local problems may respond to orthotics and stretching, whereas referred sources often require targeted spinal interventions like epidural injections. Early differentiation guides our individualized pain treatment plans, optimizing outcomes and reducing unnecessary procedures.
Referred foot pain originates from spinal conditions compressing nerves that radiate downward. Sciatica, for instance, involves irritation of the sciatic nerve root in the lumbar spine, often due to disc heriation or stenosis, leading to radicular symptoms in the foot as described in AAPM&R resources on lumbar radiculopathy. This pathway transmits burning or tingling sensations, mimicking local issues but tied to back complaints. In Bloomingdale’s aging population, spinal stenosis narrows the canal, compressing nerves and referring neuropathic pain to the sole or toes. We frequently coordinate nonsurgical therapies, such as physical therapy or radiofrequency ablation, to address these root causes effectively.
Risk factors in Bloomingdale amplify both types, including obesity, repetitive standing in service industries, and age-related spinal changes. Basic diagnostics begin with patient history and physical exams, assessing tenderness, gait, and nerve function. Imaging like X-rays or MRIs confirms spurs or compressions. Recognizing these early prevents chronicity, allowing for management through customized care at facilities like ours. Once causes are understood, exploring symptoms and diagnostics reveals more about tailored relief options.
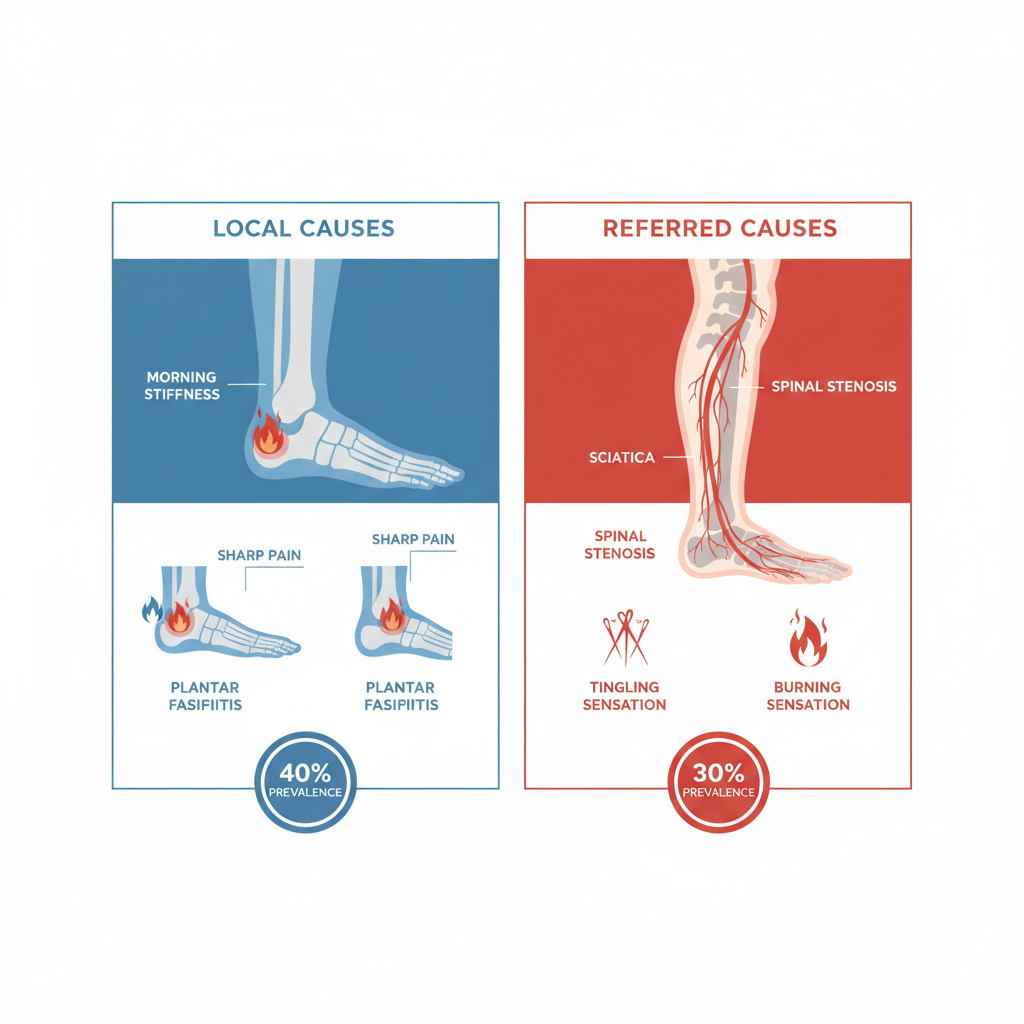
Visual breakdown of local and referred foot pain causes with key statistics
Building on this overview, the infographic above visually reinforces how local inflammation contrasts with referred nerve signals, helping readers connect personal experiences to potential diagnoses. In our experience, this educational approach encourages proactive steps toward comprehensive evaluation.
Deep Dive into Foot Pain Symptoms and Diagnosis
Symptoms provide clues to origins let’s examine them closely. In our practice at Advanced Pain & Spine Management, we frequently address foot pain in Bloomingdale, Illinois, where patients seek relief from both local and referred sources. Understanding these manifestations helps guide appropriate evaluations and individualized pain treatment plans.
Recognizing Symptoms of Plantar Fasciitis and Heel Pain
Plantar fasciitis often presents with sharp, stabbing pain in the heel, particularly upon taking the first steps in the morning. This discomfort stems from inflammation of the plantar fascia, the thick band of tissue connecting the heel bone to the toes, leading to arch stiffness and tenderness that worsens with prolonged standing or activity. Our patients often report this as a deep ache that eases somewhat with movement but returns intensely after rest, distinguishing it from general fatigue.
Heel pain variants, such as bursitis or bone spurs, share similar calcaneal discomfort indicators but may include swelling or localized redness around the heel pad. Unlike neuropathic signs from spinal issues, these local symptoms lack widespread tingling or numbness, focusing instead on mechanical aggravation. For instance, a patient in her 50s described her morning routine starting with a jolt of pain that subsided into a dull throb by midday, highlighting how fascia inflammation signs disrupt daily life.
According to a PMC article on foot pain, plantar fasciitis affects up to 10% of the population, with higher prevalence among runners and those over 40, underscoring its commonality in communities like Bloomingdale. Recognizing these patterns early allows for timely intervention, preventing chronicity. Heel pain as a sign of plantar fasciitis demands attention to activity levels and footwear, with initial self-care like stretching offering modest relief at home.
The following table contrasts key symptoms to aid differentiation between plantar fasciitis and sciatica-induced foot pain, drawn from Mayo Clinic sciatica guidelines and AAPMR symptom checklists:
| Symptom | Plantar Fasciitis | Sciatica Foot Pain |
|---|---|---|
| Heel and arch | Pain Location | Toes and sole |
| First steps in morning | Triggers | Prolonged sitting |
Diagnostic Approaches for Referred Foot Pain
When foot pain suggests a spinal origin, such as sciatica, nonsurgical evaluations form the cornerstone of our approach at Advanced Pain & Spine Management. Physical exams begin with assessing gait, reflexes, and tenderness points to differentiate local issues like plantar fasciitis from referred neuropathic symptoms, including tingling, weakness, or numbness in the toes. We correlate these with patient history, noting if discomfort radiates from the lower back, a hallmark of sciatica compressing the sciatic nerve.
Imaging plays a pivotal role; X-rays detect heel spurs or structural anomalies in plantar cases, while MRI reveals spinal sources like disc herniation causing foot symptoms. For nerve-specific insights, NCS/EMG testing measures electrical activity to confirm neuropathy, validating protocols from Mayo Clinic sciatica diagnosis guidelines. These tools help pinpoint if chronic symptoms, persisting beyond six weeks, warrant specialist referral to avoid progression.
In scenarios involving sacroiliac joint dysfunction, which can mimic sciatica with referred leg and foot pain, diagnostic injections provide both confirmation and temporary relief. Our team uses targeted injections to assess response, emphasizing their effectiveness in mapping pain pathways without surgery. In refractory cases where nonsurgical measures and diagnostic injections do not provide durable relief, surgical options such as sacroiliac joint fusion may be considered in consultation with our specialists.
To further clarify, the table below outlines common diagnostic tests and their uses:
| Treatment | Target Condition | Effectiveness | Duration |
|---|---|---|---|
| Trigger Point Injections | Plantar fasciitis | High for local relief | Temporary, 3-6 months |
| Lumbar Epidural | Sciatica foot pain | Effective for nerve inflammation | Up to 12 months |
These nonsurgical methods ensure comprehensive yet minimally invasive assessment, aligning with our commitment to customized care. With diagnosis in hand, practical management options become clear, empowering patients with targeted strategies for relief.
At Advanced Pain & Spine Management, we stress that results may vary, and this information serves as an educational guide not a substitute for professional medical advice. Consult our specialists for personalized evaluation.
Practical Non-Surgical Treatments for Foot Pain
Armed with a diagnosis, let’s explore practical steps to address foot pain in Bloomingdale, Illinois. At Advanced Pain & Spine Management, we prioritize non-surgical options that provide relief without invasive procedures. These treatments focus on reducing inflammation, strengthening supporting structures, and alleviating symptoms from conditions like plantar fasciitis and heel pain. Our individualized pain treatment plans combine expert guidance with accessible therapies to help patients regain mobility and comfort effectively.
Injections and Physical Therapy Options
For many patients experiencing plantar fasciitis or heel pain, targeted injections and physical therapy form the cornerstone of non-surgical management. We coordinate these therapies to target inflammation in the plantar fascia, the thick band of tissue along the bottom of the foot. Trigger point injections deliver corticosteroids directly into painful muscle knots, offering quick local relief. According to AAPMR guidelines, this approach is particularly effective for fasciitis management techniques, with many patients reporting reduced tenderness within days.
The procedure involves a brief outpatient visit where our specialists, like Dr. George Macrinici, use imaging guidance for precision. Benefits include minimized downtime and improved daily function, though results vary. Implementation starts with a consultation to assess suitability, followed by post-injection care such as rest and ice application.
The following table compares key non-surgical treatment options for foot pain, highlighting selection factors like condition specificity and expected relief timeline:
| Treatment | Invasiveness | Suitability for Foot Pain | Outcomes |
|---|---|---|---|
| Radiofrequency Ablation | Minimally invasive | Chronic nerve pain | Long-term relief |
| Spinal Cord Stimulation | Implant-based | Refractory sciatica | Significant reduction |
Physical therapy complements injections by building long-term resilience. Evidence-based protocols from AAPMR emphasize stretching and strengthening exercises. For instance, calf stretches involve standing facing a wall, one foot back, and leaning forward to feel the pull in the heel cord hold for 30 seconds, repeat three times daily. These fasciitis management techniques reduce tension in the plantar fascia, promoting healing over 4-6 weeks.

Infographic comparing non-surgical foot pain treatments with icons and durations
Managing Referred Pain from Spinal Issues
Foot pain stemming from spinal conditions, such as sciatica, often requires addressing the nerve root compression higher up. At our Bloomingdale location, we specialize in non-surgical options like lumbar epidural steroid injections to manage these referred symptoms effectively. This treatment targets inflammation around spinal nerves, reducing radiating pain to the foot without surgery.
The procedure entails injecting a corticosteroid and anesthetic into the epidural space via fluoroscopic guidance, typically in 15-30 minutes. Mayo Clinic data supports its efficacy, with up to 70% of patients experiencing significant relief from sciatica-related foot symptoms for 3-12 months. In cases linked to vertebral compression fractures, which can exacerbate nerve impingement, we evaluate spinal stability first.
Advanced Interventional Treatments for Persistent Foot Pain
When standard approaches fall short for foot pain in Bloomingdale, Illinois, our team at Advanced Pain & Spine Management turns to advanced interventional treatments. These minimally invasive procedures target persistent neuropathic pain, often stemming from spinal issues like sciatica or resistant lower limb pain. Radiofrequency ablation uses heat to disrupt pain signals from affected nerves, particularly effective for sciatica-related heel pain radiating to the foot.
Spinal cord stimulation involves implanting a device that delivers electrical pulses to the spinal cord, modulating pain perception in the lower extremities. For more precise targeting, dorsal root ganglion stimulation focuses on the dorsal root ganglia, key sites for foot-specific neuropathic signals. Intrathecal pumps represent another advancement, delivering medication directly to the spinal fluid for intractable sole neuropathy. Comprehensive care extends beyond the foot, providing specialized treatments like cervical dystonia treatment when necessary.
Frequently Asked Questions on Foot Pain Management
Can plantar fasciitis be cured? While a complete cure isn’t always possible, we focus on effective management with stretching, orthotics, and physical therapy to reduce inflammation and prevent recurrence.
What are home remedies for heel pain, and when should I seek help? Ice packs, rest, and supportive shoes provide relief. Consult us if pain persists beyond two weeks or includes swelling.
How is sciatica linked to foot pain, and what treatments help? Sciatica can cause radiating foot pain via nerve compression. We recommend epidural injections and physical therapy for non-surgical relief.
Are injections effective for neuropathic foot pain? Yes, targeted injections like nerve blocks reduce neuropathy symptoms by 50-70% in many cases, interrupting pain signals.
When should I see a specialist for chronic foot pain? We advise visiting if pain lasts over six weeks, limits mobility, or stems from spinal issues.
What non-surgical spinal options address foot pain? Options include radiofrequency ablation and spinal cord stimulation, similar to approaches in spasmodic torticollis management.
Taking Steps for Foot Pain Relief in Bloomingdale
Managing foot pain in Bloomingdale, Illinois, begins with understanding common causes such as plantar fasciitis, heel pain, and sciatica. At Advanced Pain & Spine Management, we emphasize a progressive approach from physical therapy and injections to advanced options like spinal cord stimulation, ensuring individualized pain treatment plans that prioritize non-surgical efficacy.
We invite you to schedule a consultation at our Bloomingdale location today for customized care tailored to your needs.
Resources
Arlington Heights
IL
60005
