Table of Contents
Understanding Pelvic Pain in Arlington Heights, Illinois
Pelvic pain in Arlington Heights, Illinois, affects many adults, disrupting daily routines and quality of life. At Advanced Pain & Spine Management, we recognize this as a persistent discomfort in the lower abdomen or pelvis lasting more than six months, often linked to gynecological, musculoskeletal, or nerve-related issues. According to StatPearls, it impacts up to 25% of women, with similar prevalence in men due to varied causes like infections or spine conditions.
Pelvic Pain Definition: Chronic lower abdominal discomfort or pelvic region aches that persists beyond six months, potentially accompanied by symptoms such as bloating, irregular bleeding, or pain during intercourse. Red flags include severe pain disrupting sleep or work, fever, unexplained weight loss, or neurological symptoms like leg weakness.
When should you seek medical help? We advise consulting a specialist promptly if pain interferes with activities or signals underlying issues, such as spine-related referrals for sciatica or stenosis. Common causes include gynecological factors like endometriosis or ovarian cysts, alongside musculoskeletal strains noted in Mayo Clinic’s overview of pelvic pain origins. Our board-certified team, led by Dr. George Macrinici, coordinates nonsurgical therapies and advanced procedures at our two convenient locations in Arlington Heights and Bloomingdale.
This guide explores fundamentals, delves into causes, and outlines treatment options. We at Advanced Pain & Spine Management offer individualized pain treatment plans focused on minimally invasive care. For insights into patient experiences, explore pain management clinic reviews. Remember, this information is educational and not a substitute for professional medical advice–consult your healthcare provider for personalized guidance.
Basics of Pelvic Pain
Pelvic pain refers to persistent or recurring discomfort in the lower abdomen or pelvis, often lasting more than six months and affecting daily activities. This condition impacts both men and women, though it is more prevalent in females, with studies indicating it affects 15-20% of women of reproductive age. At Advanced Pain & Spine Management, we recognize pelvic pain as a complex issue that can stem from various sources, including musculoskeletal, gynecological, and urological factors. Understanding its basics empowers patients to seek timely evaluation, especially when symptoms suggest underlying spine or nerve involvement.
The causes of pelvic pain are multifactorial, often involving interconnected systems like the spine, reproductive organs, and urinary tract. In adults, common origins include musculoskeletal issues such as sciatica or spinal stenosis, where nerve compression leads to radiating discomfort from the lower back to the pelvis. Gynecological conditions like endometriosis contribute to chronic inflammation and scarring in the pelvic area. Urological problems, such as bladder infections, can also trigger sharp or burning sensations. Risk factors include prior trauma, hormonal imbalances, and conditions like ovarian cysts, which may exacerbate pelvic pain in Arlington Heights, Illinois, communities where access to specialized care is essential. Addressing pelvic discomfort origins requires a thorough assessment to identify lower torso pain sources accurately.
The following table outlines common causes of pelvic pain in adults, drawing from established medical insights:
| Cause Category | Examples | Common Symptoms | Initial Evaluation |
|---|---|---|---|
| Musculoskeletal/Spine-Related | Sciatica, spinal stenosis | Pain worsening with movement | Physical exam, imaging if needed |
| Gynecological | Endometriosis, ovarian cysts | Pain during menstruation | Pelvic exam, ultrasound |
| Urological | Bladder infections | Frequent urination | Urine analysis |
This comparison highlights how diverse pelvic pain presentations demand targeted approaches. For instance, spine-related causes often overlap with broader back pain causes treatments, emphasizing the need for integrated diagnostics. Early identification through these steps can prevent progression, and we recommend multidisciplinary assessments involving pain specialists, gynecologists, and urologists to tailor solutions effectively.
Beyond the table, recognizing patterns in symptoms aids in prompt intervention. Central sensitization may amplify sensations, turning mild discomfort into chronic issues linked to comorbidities like irritable bowel syndrome or mood disorders. In our practice, we prioritize comprehensive evaluations to differentiate these factors.

Common causes and symptoms of pelvic pain in adults
Diagnosis begins with a detailed patient history and physical examination to pinpoint triggers. We employ advanced tools like NCS/EMG testing at our Arlington Heights facility to assess nerve function in spine-related cases, complemented by imaging such as ultrasounds or MRIs for gynecological or urological insights. This evidence-based protocol, aligned with clinical guidelines, ensures accurate identification without unnecessary invasiveness.
Red Flags for Pelvic Pain
Seek immediate care if you experience severe pain with fever, unexplained weight loss, blood in urine or stool, or sudden inability to pass urine or stool. These may indicate serious conditions requiring urgent attention.
Preventive strategies focus on lifestyle adjustments to mitigate risk. Maintaining good posture reduces spinal strain, while regular exercise strengthens pelvic floor muscles. Weight management and stress reduction through mindfulness can lessen flare-ups, promoting overall well-being in line with our individualized pain treatment plans.
Exploring Causes and Diagnosis of Pelvic Pain
Chronic pelvic pain affects many individuals, often stemming from a variety of gynecological, musculoskeletal, or neurological sources. At Advanced Pain & Spine Management, we specialize in identifying these underlying factors through comprehensive evaluations tailored to each patient’s needs. Understanding the specific causes allows for more precise interventions, particularly in our community dealing with pelvic pain in Arlington Heights, Illinois.
Detailed Causes Including Endometriosis and Ovarian Cysts
Gynecological conditions frequently contribute to pelvic pain, with endometriosis and ovarian cysts being prominent examples. Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus, leading to inflammation and scarring. Symptoms often include cyclical pain that worsens during menstruation, heavy periods, pain during intercourse, and fatigue. According to StatPearls, this condition affects up to 10% of reproductive-age women and can become chronic due to central sensitization in the nervous system, making pain more intense over time.
Endometriosis Overview
Endometriosis is characterized by endometrial tissue disorders causing adhesions and lesions. It often presents with dysmenorrhea, dyspareunia, and infertility. Diagnosis challenges arise from overlapping symptoms with other disorders, requiring careful history-taking to differentiate.
Ovarian cysts, fluid-filled sacs on the ovaries, can cause sharp or dull pelvic discomfort, especially if they grow large or rupture. Signs of a ruptured ovarian cyst include sudden severe pain, nausea, and lightheadedness, which may mimic other emergencies. Most cysts resolve on their own, but persistent ones may require monitoring or surgical removal. Diagnostic challenges involve distinguishing benign cysts from those linked to conditions like polycystic ovary syndrome, as noted in Mayo Clinic resources on chronic pelvic pain.
Ovarian Cyst Signs
Cyst-related discomfort may include bloating, irregular bleeding, and pressure on the bladder or bowels. Rupture risks increase with physical activity, necessitating prompt evaluation to rule out complications like torsion.
Spine-related causes, though less obvious, can refer pain to the pelvis via nerve pathways, complicating initial assessments. These multifaceted etiologies underscore the need for multidisciplinary approaches to pinpoint the source effectively.
Diagnostic Methods for Chronic Pelvic Pain
Diagnosing chronic pelvic pain begins with a thorough medical history and physical examination, focusing on pain patterns, associated symptoms, and potential triggers. We utilize a step-by-step approach, starting with pelvic exams to assess tenderness or abnormalities, followed by laboratory tests to check for infections or hormonal imbalances. Imaging plays a crucial role, with ultrasounds providing quick views of reproductive organs and MRIs offering detailed insights into soft tissues and potential adhesions.
Personalized diagnosis is key, as no single test fits all cases. Choosing the right diagnostic tools depends on the suspected cause, ensuring efficiency while minimizing patient discomfort. The following table compares approaches for common pelvic pain etiologies, highlighting their strengths and local accessibility.
| Cause | Primary Diagnostic Tool | Accuracy/Pros | Local Availability Notes |
|---|---|---|---|
| Endometriosis | Laparoscopy, ultrasound | High specificity for lesions | Coordinated with gynecology in Arlington Heights |
| Ovarian Cysts | Pelvic ultrasound, MRI | Non-invasive, quick results | Routine at local clinics like ours |
| Spine/Nerve Related | MRI spine, NCS/EMG | Identifies nerve compression | Offered at Advanced Pain & Spine Management |
These results guide treatment by clarifying the pain’s origin, allowing us to integrate findings into individualized pain treatment plans. For instance, confirming endometriosis might lead to hormonal therapies, while nerve issues could prompt targeted blocks. Sourced from Mayo Clinic and NICHD guidelines, this structured evaluation ensures comprehensive care, reducing diagnostic delays and improving outcomes for patients in our practice.
Specialist evaluations, including referrals to gynecologists or neurologists, enhance accuracy. In Arlington Heights, we coordinate these seamlessly, often incorporating advanced testing like nerve conduction studies to address overlapping symptoms effectively.
When Spine or Nerve Issues Contribute to Pelvic Pain
Pelvic pain can sometimes originate from spine or nerve problems, such as herniated discs or cluneal nerve irritation, which refer discomfort to the lower abdomen. These neurological connections amplify pain through pathways like the pudendal or ilioinguinal nerves, often exacerbated by poor posture or trauma. Symptoms may include radiating pain, numbness, or weakness in the legs, mimicking gynecological issues.
We utilize NCS/EMG testing to evaluate nerve function and detect compression or neuropathy accurately. This evidence-based method, as outlined in interprofessional guidelines, helps differentiate spine-related causes from others. Once identified, options like pain conditions treatments including nerve blocks provide relief. Addressing these contributions early prevents chronicity, aligning with our commitment to customized care at Advanced Pain & Spine Management.
Treatment Options for Pelvic Pain
At Advanced Pain & Spine Management, we specialize in developing individualized pain treatment plans for pelvic pain, drawing on evidence-based strategies to address underlying causes such as endometriosis, ovarian cysts, and spine-related issues. Our approach begins with conservative measures and progresses to advanced interventions as needed, ensuring customized care at our Arlington Heights and Bloomingdale locations. By coordinating multidisciplinary therapies, we help patients achieve effective pelvic disorder management while minimizing risks.
Nonsurgical and Minimally Invasive Therapies
We prioritize nonsurgical and minimally invasive therapies as the foundation of pelvic pain treatment, tailoring options to the specific cause identified during diagnosis. Physical and occupational therapy coordination plays a central role, focusing on pelvic floor strengthening to alleviate muscle spasms and improve function, as supported by FDA insights on the benefits of targeted exercises for pelvic health. Medication management includes pain relievers, muscle relaxants, and antidepressants to control symptoms, with hormonal therapies added for gynecological contributors. For many patients, these cause-specific interventions provide substantial relief without invasive procedures.
Personalized selection of therapies depends on pain intensity, frequency, and etiology. According to NICHD guidelines, starting with conservative options like physical therapy and medications yields success rates of up to 70% for musculoskeletal pelvic pain, allowing us to monitor progress before escalating.
| Treatment Type | Examples | Benefits | Suitability for Causes |
|---|---|---|---|
| Injections | Sacroiliac joint, nerve blocks | Targeted inflammation reduction | Spine/nerve, SI joint pain |
| Stimulation Therapies | Spinal cord, dorsal root ganglion | Long-term management | Neuropathic pelvic pain |
| Botox Injections | For spasticity overlap | Muscle relaxation | Spasticity-related pelvic issues |
Following these treatments, recovery expectations vary but often involve minimal downtime. Mayo Clinic data indicates that injections provide relief within days, with most patients resuming activities in 24-48 hours under our guided protocols. We integrate physical therapy post-procedure to enhance outcomes and prevent recurrence, emphasizing our commitment to comprehensive, minimally invasive pain treatments.
Our team coordinates these therapies seamlessly, offering quick access to board-certified specialists like Dr. George Macrinici for optimal results in pelvic pain management.
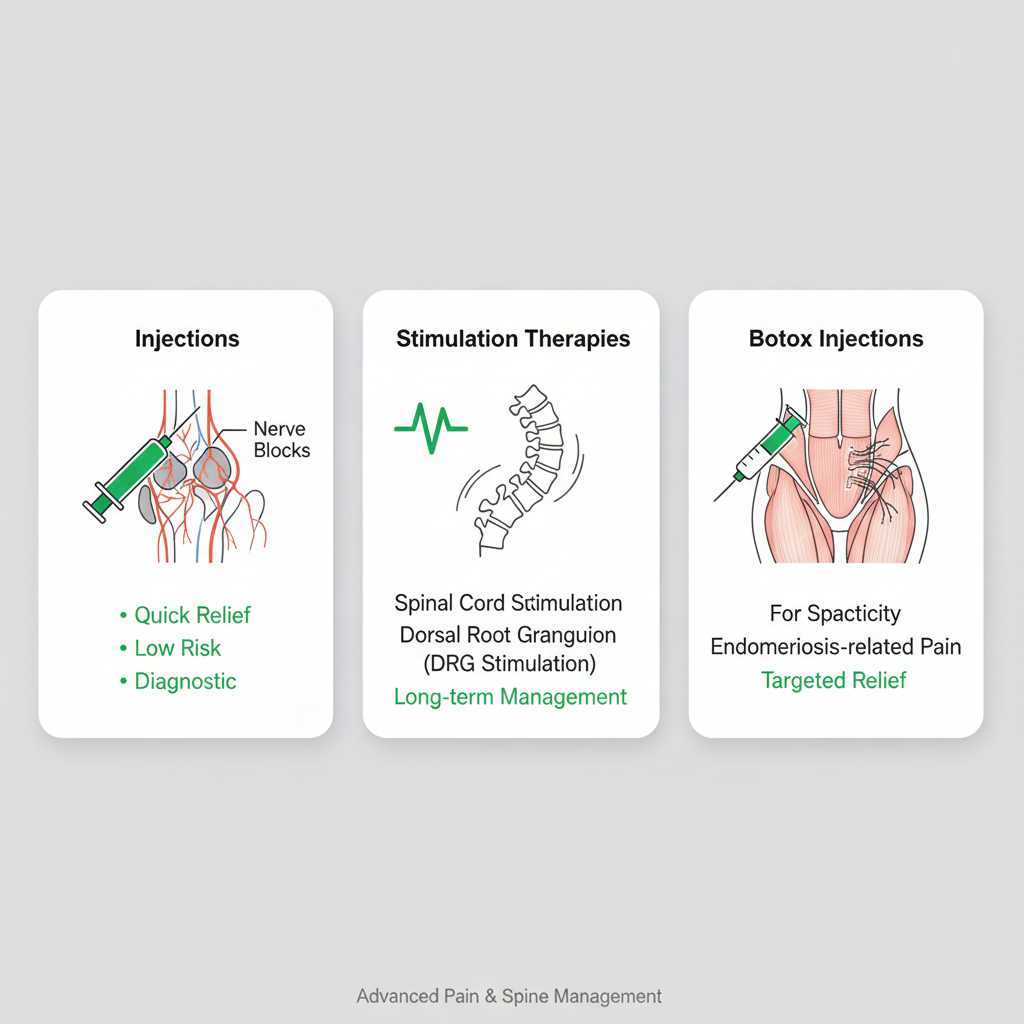
Minimally invasive treatment options for pelvic pain visualized
This visual overview highlights how we select therapies based on patient needs, bridging nonsurgical approaches with more targeted care for sustained relief.
Local Treatments for Endometriosis and Ovarian Cysts
For patients experiencing pelvic pain in Arlington Heights, Illinois, we offer specialized treatments for endometriosis and ovarian cysts through close collaborations with gynecological experts. Hormonal therapies, such as birth control pills or progestin-releasing devices, effectively manage endometriosis symptoms by reducing inflammation and tissue growth, as outlined in NICHD recommendations. When cysts contribute to discomfort, we monitor via ultrasound and initiate pain medication management alongside lifestyle adjustments like dietary changes to alleviate pressure.
In cases requiring escalation, we facilitate referrals for minimally invasive laparoscopic procedures to remove cysts or excise endometrial tissue, prioritizing preservation of fertility where possible. Our individualized pain treatment plans incorporate occupational therapy to address daily impacts, ensuring holistic pelvic disorder management. For endometriosis-related pelvic pain in Arlington Heights, timely intervention prevents progression, with our Advanced Treatments providing rapid symptom control. We also guide patients on when to see a doctor for ovarian cyst pain, such as sudden severe episodes warranting immediate evaluation.
These local options reflect our unique selling points, including convenient access and multidisciplinary coordination for effective, evidence-based care.
Addressing Spine and Nerve-Related Pelvic Pain
Spine and nerve-related pelvic pain often stems from neuropathic components, such as sciatica or sacroiliac dysfunction, which we address through targeted procedures. Nerve blocks, including ilioinguinal and superior hypogastric plexus blocks, deliver precise anesthesia to interrupt pain signals, offering diagnostic insights alongside relief. For refractory cases, consider neuromodulation via spinal cord stimulation or dorsal root ganglion stimulation, which modulates nerve activity for long-term management.
Nerve Block Basics: This outpatient procedure involves injecting anesthetic near affected nerves under imaging guidance. Benefits include immediate pain reduction lasting weeks to months, with low complication rates. We perform these at our facilities to confirm pain sources before advancing to back pain management options.
Radiofrequency ablation follows successful blocks to disrupt nerve conduction enduringly. Our experienced team, including Jason McAloon, DO, crafts these plans to integrate with overall therapy, bridging to specialized care for optimal outcomes.
Advanced Interventions for Pelvic Pain
When conservative measures fail to alleviate persistent pelvic pain, advanced interventions offer targeted relief for underlying nerve or structural issues. We specialize in these sophisticated approaches at Advanced Pain & Spine Management, focusing on spine and nerve-related variants that contribute to discomfort in the pelvic region. Our board-certified team employs evidence-based techniques to improve quality of life for patients dealing with refractory symptoms.
Spinal cord stimulation and dorsal root ganglion stimulation represent key options for neuropathic pelvic pain. These neuromodulation devices deliver electrical impulses to disrupt pain signals along the spinal pathways, providing substantial relief for conditions resistant to medications. For patients experiencing pelvic pain in Arlington Heights, Illinois, we implant spinal cord stimulators to modulate aberrant nerve activity effectively. Intrathecal pumps deliver medications directly to the spinal fluid, bypassing systemic side effects and offering precise dosing for chronic cases. Radiofrequency ablation targets specific nerves with heat to interrupt pain transmission, while vertebroplasty stabilizes vertebral fractures that may compress nerves leading to pelvic referral pain. Botox injections address spasticity overlaps, similar to applications in cervical dystonia treatments, by relaxing overactive muscles contributing to discomfort.
Neuromodulation Explained
Neuromodulation alters nerve activity through implanted devices, drawing from NICHD guidelines on individualized pain management. It targets the mechanism of chronic pain signaling without invasive surgery, emphasizing safety in pelvic floor care as noted by FDA resources.
Patients typically advance to these interventions after exhausting first-line therapies like physical therapy and oral medications, particularly when pain stems from endometriosis or ovarian cysts causing nerve irritation. Candidacy involves comprehensive evaluation, including imaging and nerve studies, to confirm suitability and minimize risks.
The following table contrasts advanced procedures with conservative options for managing chronic pelvic pain:
| Approach | Examples | Duration of Relief | Invasiveness Level |
|---|---|---|---|
| Conservative | Therapy, medications | Short-term (weeks) | Low |
| Interventional | Spinal cord stimulation | Long-term (months-years) | Moderate |
| Surgical Referrals | Kyphoplasty for fractures | Variable | Higher |
This comparison highlights escalation from low-risk basics to targeted neural therapies, ideal for spine or nerve-driven issues like neuropathic pelvic pain from endometriosis management or compression-related discomfort in ovarian cyst complications. Supporting data from FDA and Mayo Clinic underscore the long-term benefits of interventional methods for select patients.
At our practice, patient selection prioritizes those with confirmed diagnoses and failed conservative trials. We collaborate with specialists to tailor plans, ensuring follow-up monitoring for optimal outcomes. Benefits include reduced reliance on opioids and enhanced daily function. For accessible advanced pain modulation in Arlington Heights, our team provides these services conveniently, integrating physical therapy coordination for holistic care.
Frequently Asked Questions About Pelvic Pain
What are the symptoms of endometriosis causing pelvic pain?
Endometriosis often leads to chronic pelvic pain, painful periods, pain during intercourse, and heavy menstrual bleeding. According to Mayo Clinic, these symptoms arise from tissue similar to the uterine lining growing outside the uterus, affecting daily activities for many women.
What are the signs of a ruptured ovarian cyst?
Signs include sudden, sharp pelvic pain, bloating, nausea, and sometimes fever or vomiting. Mayo Clinic notes that ovarian cysts commonly cause discomfort, but rupture requires prompt evaluation to prevent complications like infection.
Can spine issues contribute to pelvic pain?
Yes, conditions like spinal stenosis or herniated discs can refer pain to the pelvic area through nerve pathways. We address these connections in our individualized pain treatment plans at Advanced Pain & Spine Management.
When should I seek help for pelvic pain related to ovarian cysts?
Seek immediate care if pain is severe, accompanied by dizziness, rapid breathing, or fever. Early intervention helps manage ovarian cysts effectively and avoids escalation.
How can I access specialists for pelvic pain in Arlington Heights, Illinois?
Local options include pain management clinics offering minimally invasive treatments. We can assist with evaluations tailored to pelvic pain in Arlington Heights, Illinois, focusing on comprehensive care.
For personalized advice, consult a specialist to discuss your symptoms.
Managing Pelvic Pain Effectively in Arlington Heights
In summary, effective management of pelvic pain in Arlington Heights, Illinois, begins with identifying common causes such as endometriosis, ovarian cysts, and spine-related issues. At Advanced Pain & Spine Management, we emphasize early intervention through comprehensive diagnostics and individualized treatment pathways, including our minimally invasive options that prioritize patient comfort and recovery.
We invite you to consult our experienced team for tailored plans that address your unique needs, empowering you to reclaim your quality of life with evidence-based pelvic health strategies. As the FDA highlights in guidance on pelvic floor health, incorporating simple maintenance exercises can support long-term wellness and prevent flare-ups.
Drawing from our expertise in conditions like spasmodic torticollis management, we remain committed to holistic pain relief.
Resources
Arlington Heights
IL
60005
